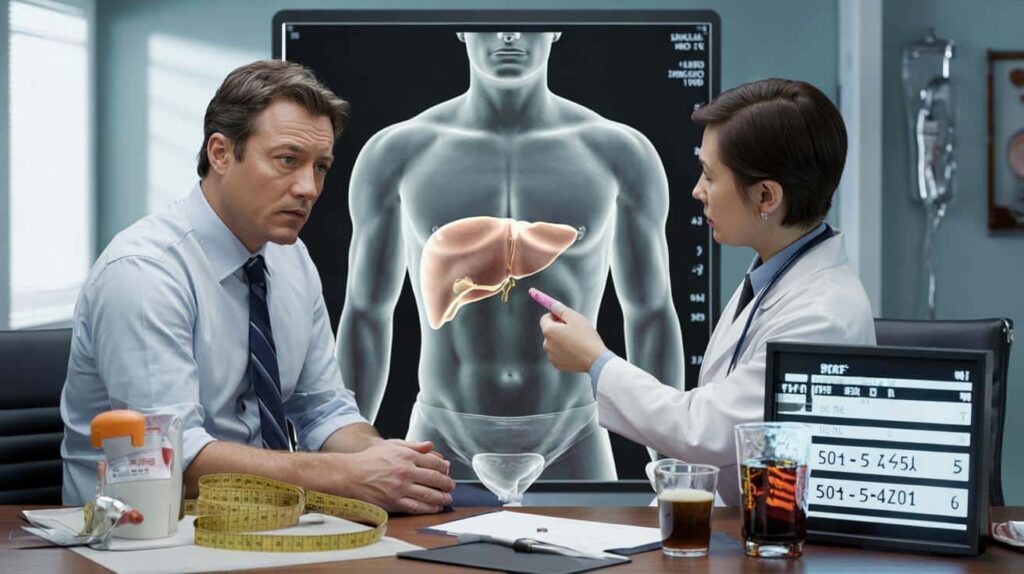
The waiting room was quiet except for the soft buzz of a vending machine and the nervous rustle of paper forms. Next to me, a man in his forties kept glancing at his phone, then at the door, one knee bouncing non-stop. He didn’t “look” sick. Slight belly, office shirt, wedding ring. The kind of person who tells you he’s just tired from work.
When the hepatologist finally called his name, he stood up with that half-smile people use when they’re trying not to be scared. Ten minutes later he came back out, eyes a bit stunned, clutching a sheet of paper: fatty liver disease. No symptoms he’d taken seriously. No pain. Just a silent organ quietly drowning in fat for years.
Six warning signs your liver is quietly struggling
Most people imagine liver disease as something loud and obvious: yellow eyes, intense pain, dramatic hospital scenes. Fatty liver doesn’t play that game. It advances slowly, silently, disguised as normal tiredness weight gain, busy-life aches. That’s exactly why hepatologists keep repeating the same sentence: you can have a seriously overloaded liver and still feel more or less ok.
 The Ordinary serum called filler in a bottle gives skin smoother youthful appearance in your 40s
The Ordinary serum called filler in a bottle gives skin smoother youthful appearance in your 40s
The first sign many of them notice, especially in their overweight or sedentary patients, is a deep dragging fatigue that doesn’t match the day they’ve had. Not a one-night-bad-sleep tired, but a background exhaustion that just never leaves. The kind where you wake up already wanting to go back to bed.
That’s the trap: when almost everyone around you is tired and gaining belly fat, abnormal starts to feel normal.
From a medical standpoint, fatty liver is simple and brutal. The liver starts accumulating fat inside its cells, often linked to insulin resistance sugary drinks, frequent snacking, ultra-processed foods, lack of movement. Over time, the organ inflames. Cells get damaged. Scars appear. What was just fatty liver can become steatohepatitis, then fibrosis, then full-blown cirrhosis.
The body tries to send quiet alerts. Mild discomfort in the right upper abdomen. Unexplained brain fog. A strange heaviness after meals. Sometimes subtly darker under-eyes, or a feeling of being puffy None of these scream emergency, so people ignore them for years.
The six overlooked signs hepatologists keep seeing
The first sign many patients shrug off is that deep ongoing fatigue that doesn’t improve with sleep. Hepatologists explain that when the liver is overloaded with fat, it doesn’t manage energy and toxins as efficiently. You might feel like you’re moving through mud, mentally and physically, especially in the afternoon. That’s not just getting older.
Second, there’s the belly. Not generic weight gain everywhere, but a thickening waist that rounded abdomen that feels new, tight jeans where they used to be comfortable. Doctors regularly see people with relatively normal overall weight but a pronounced abdominal fat and fatty liver on ultrasound. Visceral fat the one hugging your organs, loves to travel with liver fat.
Third warning sign: slightly altered blood tests, casually dismissed Numbers. A mild rise in ALT or AST enzymes, a bit of elevated triglycerides Numbers that don’t panic anyone, until you put them in the context of the whole picture.
The fourth sign is more subtle: feeling heavy or bloated after relatively small meals, especially rich or sugary ones. Not sharp pain, just a persistent fullness sometimes with vague discomfort on the right side under the ribs. Many patients chalk it up to I eat too fast or my digestion is weird lately. A hepatologist will tell you they see this pattern almost every day.
Fifth, brain fog. People report trouble concentrating forgetting simple things, needing more time to get going mentally. The liver plays a role in clearing substances from the blood that, when they accumulate, can affect the brain. You won’t necessarily link a scattered mind to your liver, yet the connection is real.
Finally, the sixth sign: small changes in the skin and general appearance. Duller skin itching without rash, easy bruising, or these small red spider-like blood vessels on the chest or face. On their own, they’re not dramatic. Together, they can sketch the outline of a struggling liver.
A specialist I interviewed summed it up in one line: fatty liver is often a lifestyle mirror. It reflects years of habits liquid calories, late-night snacking, sitting too long, never really recovering from stress. That’s not a moral failing it’s just the way modern life is built.
How to react when these signals ring a small alarm
The first concrete step isn’t heroic. It’s booking a simple check-up with your doctor and asking directly for liver function tests and, if needed, an ultrasound. You don’t need to arrive with a perfect speech Just describe what you feel: the fatigue that won’t leave, the belly that changed, the brain fog that surprises you, that weird fullness after meals.
Doctors are used to this. Many will also look at your waist circumference blood pressure, blood sugar, lipids. The goal is not to label you but to see the bigger picture: metabolic health and liver health go hand in hand. A basic panel of tests can already tell a lot.
For some people, that appointment is the first time someone connects their daily life with what’s happening inside their liver.
Once the alarm has sounded, the most effective gestures are surprisingly ordinary. Cutting back on sugary drinks juices energy drinks, and alcohol. Eating real meals instead of constant grazing Adding 20–30 minutes of walking on most days, not as a performance, but as a new baseline.
This is where a lot of guilt and frustration shows up. People feel they should have known, should have eaten better, should have moved more. A good hepatologist usually stops that spiral quickly The reality is that the world is organized around screens, chairs, and ultra-processed food. Of course the liver ends up paying the price.
You don’t need a perfect lifestyle. You need a slightly better one, consistently. And that already changes the liver’s future.
Fatty liver is one of the few chronic diseases we actually see improve on scans, says one hepatologist. When patients change small things less sugar, fewer processed foods, more walking the fat in the liver can decrease. We literally see the organ breathe again.
Listen to persistent fatigue
If your tiredness feels disproportionate to your days, especially with brain fog and low energy, don’t just blame your personality or age. Ask for a blood test that includes liver enzymes.
Watch your waist, not just your weight
A growing belly, even at a normal BMI is a red flag for visceral fat and possible liver overload. A tape measure around your waist can be more honest than the bathroom scale.
Act on small daily levers
Swapping one sugary drink per day for water, walking after dinner, and spacing your meals can sound boring, yet these are the habits hepatologists see in patients whose liver slowly gets back on track.
Liver health as a quiet wake-up call
Fatty liver disease is rarely the story of one bad decision. It’s the sum of hundreds of small understandable choices: the elevator instead of the stairs, the dessert at the desk, the late glass of wine to unwind, the skipped check-up because the calendar was already full. The liver loyal and silent, absorbs it all until it begins to protest in its own low-key way.
Many people only discover the problem by accident, during a routine ultrasound a work check-up, or a fertility assessment. Some feel betrayed by their own body. Others feel lucky to have caught it early enough The truth sits somewhere between those two emotions.
When a hepatologist lists the six subtle warning signs chronic fatigue, abdominal weight gain, altered blood tests, post-meal heaviness, brain fog, skin changes it’s not to scare anyone. It’s an invitation to reconnect with a part of the body that doesn’t speak loudly.
Talking about it with friends or family often reveals the same pattern Oh I have that too. I thought it was just stress. That exchange, around a table or in a WhatsApp group, can be the first real prevention act. The liver doesn’t ask for perfection. It asks to be noticed before it’s too late.
| Key point | Detail | Value for the reader |
|---|---|---|
| Early, subtle signs matter | Fatigue, belly fat, brain fog, and mild digestive discomfort can reflect liver overload long before serious disease | Helps you take signals seriously instead of normalizing them as just stress or aging |
| Simple tests can reveal a lot | Basic blood tests and an ultrasound often detect fatty liver with no invasive procedures | Gives a clear, accessible path to check your own liver status with your doctor |
| Small lifestyle shifts are powerful | Reducing sugary drinks and alcohol, moving more, and spacing meals can reduce liver fat | Shows that real improvement is possible without extreme diets or punishing routines |
FAQ:
Is fatty liver always linked to alcohol?
No. Many cases are non-alcoholic fatty liver disease, tied to diet, sedentary lifestyle, overweight, or metabolic issues. You can have fatty liver even if you barely drink.
Can fatty liver actually reverse?
Yes, especially in early stages. With weight loss even 5–10%, better food choices, and more physical activity, doctors often see liver fat decrease on follow-up scans.
Does fatty liver always cause pain?
No. Many people feel no pain at all. Some describe a vague heaviness or discomfort under the right ribs, but absence of pain does not mean absence of disease.
What tests should I ask my doctor for?
You can ask about liver enzymes ALT AST GGT, triglycerides, fasting glucose, and, if there’s suspicion, an abdominal ultrasound to visualize the liver.
Can thin people have fatty liver?
Yes. Even people with a normal BMI can develop fatty liver, especially if they have high sugar intake, little physical activity, or metabolic risk factors like prediabetes.