When living with cancer means always being in pain
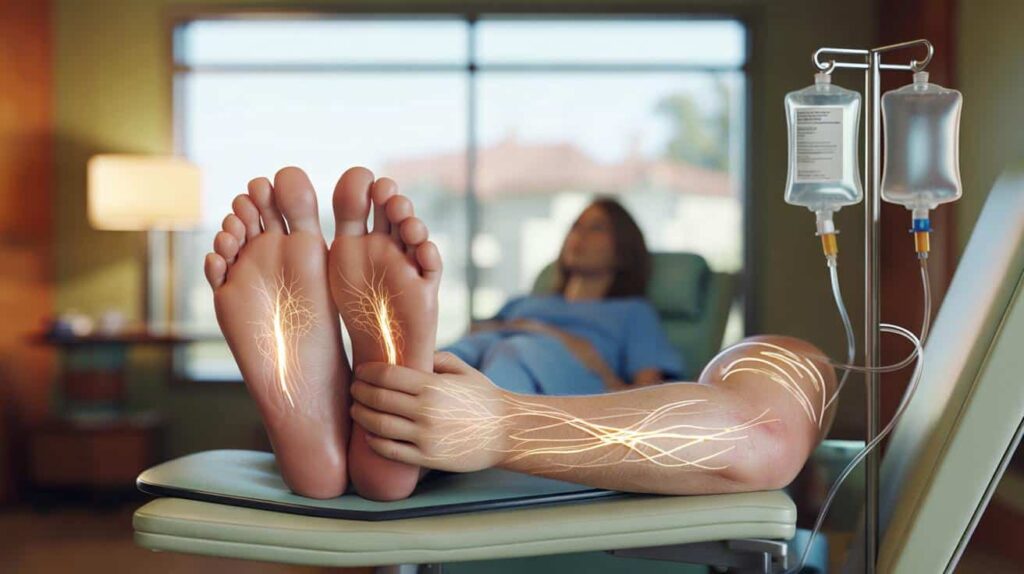
For a lot of people who have finished chemotherapy, the end of treatment doesn’t bring the clean break they were hoping for. The tumour may be gone, scans may look good, and hair may slowly start to grow back. Still, every step can feel like walking on broken glass, and every touch can hurt pain.
Chemotherapy-induced peripheral neuropathy, or CIPN, is what causes these feelings most of the time. Some cancer drugs hurt the long, thin nerves that go from the spinal cord to the hands and feet. Patients say they feel pins and needles, burning, electric shocks, or a deep, dull numbness that makes it hard to button a shirt or feel the ground.
Some common chemotherapy regimens can cause peripheral neuropathy in up to 90% of patients while they are being treated.
When neuropathy gets really bad, oncologists sometimes have to lower doses or put off cycles. That can make the whole treatment less effective against cancer and put doctors in a tough spot between keeping the disease under control and keeping the patient functioning normally.
The long-lasting effects of chemotherapy-induced neuropathy
People usually think that the side effects of chemotherapy will go away after the treatment is over. Usually, nausea goes away, taste comes back, and fatigue gets better. Neuropathy is not the same. It can take a very long time for damaged nerves to heal, if they even do.
Research shows that about one in four people with neuropathic symptoms still have them months or even years after their last drip. Some people wake up every morning with the same burning feet that started during their infusions. Some people have trouble with small motor skills, drop things, or feel unsteady on stairs.
Neuropathy is a daily reminder for those survivors that they used to have cancer, even when doctors talk about remission or cure.
Few tools, uncomfortable tricks
There aren’t many good ways to stop nerve damage from chemotherapy right now. A lot of centers now use cold gloves and socks during infusions. The goal of the technique is to narrow blood vessels and lower the amount of drug that gets to peripheral nerves by cooling the hands and feet.
But the method has some problems:
- The cold is often very uncomfortable and hard to deal with for hours.
- The results are very different for each patient.
- Even when people follow the rules strictly, some still get neuropathy.
Doctors can give patients painkillers, including some that are used to treat epilepsy or depression, to block nerve signals. These drugs can help with burning or shooting pain, but they don’t usually bring back normal feeling. Drowsiness and dizziness are two side effects that make things even harder.
At this time, there is no widely accepted and effective way to stop chemotherapy-induced peripheral neuropathy from happening.
A French lead: the Carba1 molecule
A group of researchers in France, working with people from the US and France, has found a molecule that could finally change the balance. Carba1 is the name of the compound, and it is part of a group of chemicals called carbazoles.
Carbazoles are organic molecules that have three rings in their structure. Researchers and chemists at the Centre for the Study and Research on Medicines in Normandy (CERMN) have been working on them for more than ten years. Their goal is to create small molecules that bind to biological targets that are important for nerve survival and cancer growth.
Carba1 came out of this program as a good candidate. In preclinical studies, the molecule seemed to shield nerve cells from the harmful effects of some chemotherapy drugs.
Carba1 not only protected neurones in experimental models, but it also appeared to augment the anti-tumor efficacy of certain chemotherapy agents.
What could Carba1 do to protect nerves?
Researchers are still figuring out how it works, but early studies have given us a few hints:
- Stress buffering: Carba1 seems to stop cells from responding to stress in ways that hurt nerve fibres.
- Mitochondrial support: It might help keep mitochondria, the tiny power plants inside neurones that some chemotherapy drugs hurt, working well.
- Controlling inflammation: The molecule might stop inflammatory cascades that make nerve damage worse.
These combined actions may elucidate the observed phenomenon whereby nerve cells subjected to both chemotherapy and Carba1 exhibit diminished signs of degeneration compared to those exposed solely to chemotherapy in the laboratory setting.
Instead of making cancer treatment less effective, making it better
One of the biggest worries about drugs that protect nerves is that they might also protect tumour cells, which would make chemotherapy less effective. That risk has stopped a number of potential candidates in the past.
Carba1 is different because early data point to the opposite effect. Adding the molecule to standard chemotherapy made some models kill more cancer cells. That suggests a good double action: keeping healthy neurones alive while putting more stress on cancer cells.
 No More Hair Dye New Natural Trend Covers Grey Hair Beautifully While Helping People Look Younger
No More Hair Dye New Natural Trend Covers Grey Hair Beautifully While Helping People Look Younger
A drug that protects nerves and makes chemotherapy stronger could let doctors keep giving full doses of treatment without hurting patients’ long-term quality of life.
This idea is still just a theory, but it fits well with what oncologists say they need to do their jobs every day.
What the research says
The most recent results, which were published in the journal Science Advances, come from research that was done before clinical trials. That means that most of the evidence comes from cell cultures and animal models, not people yet.
Before Carba1 can be used in clinics, there are a few things that need to happen:
| Stage | Goal |
|---|---|
| Toxicity studies | Check that Carba1 is safe at realistic doses in animals. |
| Phase 1 trials | Evaluate safety and dosing in a small group of volunteers or patients. |
| Phase 2 trials | Test early signals of nerve protection and possible impact on tumour response. |
| Phase 3 trials | Confirm benefits and risks in larger, diverse patient groups. |
It usually takes years to go down this path. But strong preclinical signals, along with the fact that it could protect nerves and fight cancer, will probably get the attention of both public funders and drug companies.
What this might mean for patients
If future human trials confirm the early promise of Carba1, it could have a big impact on how cancer is treated. Patients taking neurotoxic drugs like some platinum compounds, taxanes, or vinca alkaloids could take Carba1 with their chemotherapy.
The goal was to have fewer dose cuts, less severe sensory problems, and a lower chance of long-term pain. These are not small things for someone who is trying to work, take care of kids, or just walk without worrying about falling.
This method might be especially helpful for younger patients who have a long life ahead of them. Protecting their nerves during treatment could mean decades of better mobility, balance, and sensory function.
Understanding peripheral neuropathy in simple terms
It can be hard to understand peripheral neuropathy, so it’s helpful to think about how it affects your daily life. Think about how hard it would be to feel coins in your pocket if your fingers felt like they were wrapped in thick rubber. Or trying to drive when you can’t tell how hard your foot is pushing the pedal.
Neuropathy can cause more than just pain:
- Loss of reflexes in the wrists and ankles.
- Having trouble accurately sensing heat or cold, which makes burns more likely.
- Having trouble keeping your balance, especially at night or on uneven ground.
- Hands that cramp or feel weak, making it harder to write and cook.
Nerves take a long time to heal, so any damage done during a few months of chemotherapy can last for many years.
Patients can ask their doctors practical questions.
Carba1 isn’t available to the public yet, but people who already have neuropathy can still ask their oncology team specific questions. For instance:
- Are there any clinical trials going on right now that I could join that are looking at protecting nerves?
- Which of my chemotherapy drugs is most likely to cause neuropathy?
- When would you think about changing my dose because of nerve symptoms?
- Could occupational or physical therapy help me deal with my current symptoms?
Teams can keep track of changes over time by bringing up these issues early instead of waiting until the damage is bad.
Risks, benefits, and possible future combinations
There is always a risk with any drug. We need to carefully look at Carba1 to see if it has any side effects, interacts with other treatments, or has rare toxicities that only show up when a lot of people are exposed to it.
Scientists are also thinking about how this type of molecule could work with other helpful strategies. Cold gloves, balance-focused exercise programs, and nutritional strategies targeting nerve health may still be beneficial. A future protective package could include a drug like Carba1 and physical measures that are specific to each patient’s treatment plan.
Carba1 is still just a research story for now, not a prescription. But it shows a change in how people think about cancer care: it fights harder against tumours and doesn’t accept chronic nerve damage as the cost of survival.